Generations of Impact
Generations of Impact: Where Nursing Education Meets Real-World Change for Patients, Communities, and Policy
There is a thread that runs through Duke University School of Nursing, one that weaves together education and experience to create a tapestry of care across the lifespan. Our students, staff, faculty, and thousands of alumni have built a culture of care that has impacted countless lives in our own backyard here in Durham, across the nation, and throughout the world. Duke-trained nurses continue to lead in hospitals, clinics, schools, community programs, and anywhere care is needed.
In the article ahead, you’ll follow that thread across lifetimes and geography, meeting the people and ideas behind a spectrum of initiatives and research programs: from discoveries that reshape practice, to innovative training models, to partnerships that expand access and equity. Together, their work adds up to something larger than any single encounter— generations of impact, felt one patient, one family, and one community at a time.
For many of us, our first encounter with a nurse comes before we’ve ever seen the light of day, with maternal healthcare making a world of difference in the lives of newborns. Jessica Covil-Manset, Communications Manager at the School of Nursing, had a firsthand experience with how our Women’s Health Nurse Practitioner students are trained when she volunteered to be a pregnant model while carrying her first child.
Women’s Health Ultrasound Training: A Pregnant Person’s Account
By Jessica Covil-Manset
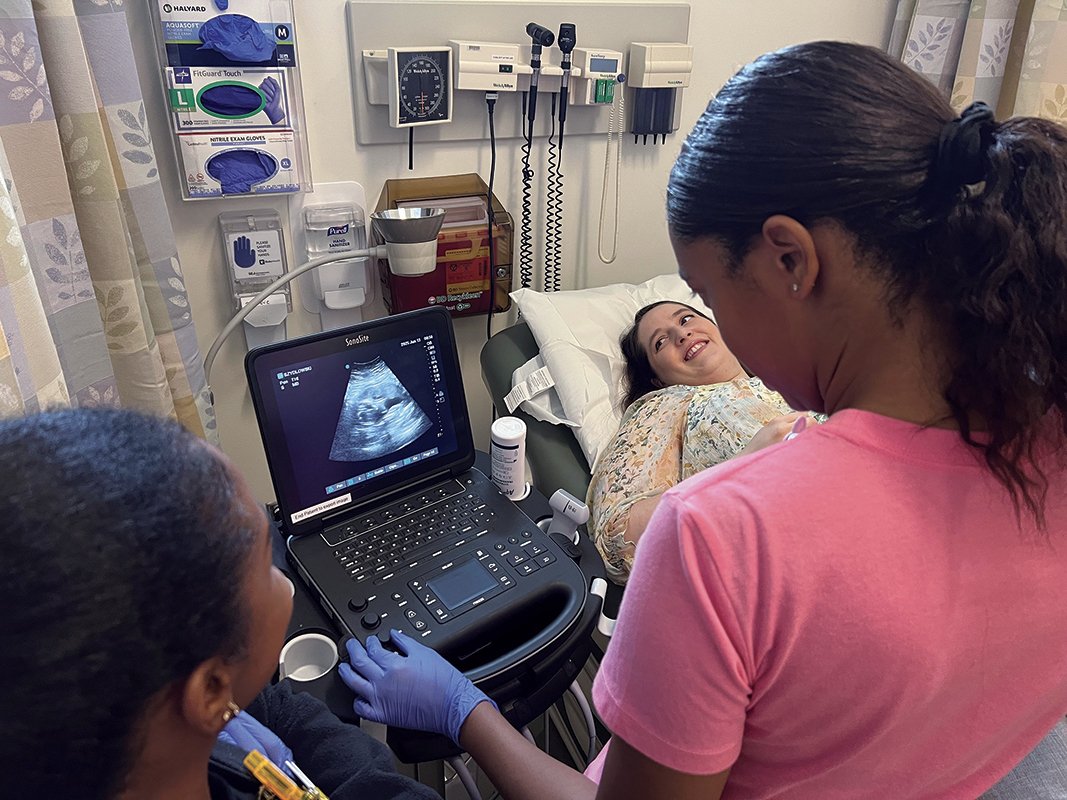
In June 2025, I volunteered to support the School of Nursing’s Women’s Health Nurse Practitioner MSN students in two perinatal ultrasound learning experiences. As the School’s Communications Manager, and with a Duke graduate background in women’s and feminist studies, I relished the opportunity to support women’s health nursing education (and to see my developing baby).
This training allowed students to conduct perinatal ultrasounds on real-life pregnant persons with a practicing technician guiding students through the basics of manipulating a transducer probe across a pregnant belly and understanding what is shown on the display screen. Students gained hands-on experience positioning and angling the probe so that it shows various parts of the uterus and the fetus, finding the placenta, the head, the spine, and the heart.
One student who participated in my ultrasound, Alexis Jordan, has been an RN since 2021, and all her nursing experience is in labor and delivery. She said that she decided to pursue her WHNP at Duke because she wanted to be more hands-on with reproductive care across the lifespan.
“So many women of all ages have had negative experiences when it comes to receiving obstetrical and gynecological care,” said Jordan. “I want to be able to improve that experience. I chose Duke due to the prestige and the location. I’m an NC native and didn’t want to be too far from home.”
Another WHNP student, Jocelin Maxwell, who engaged with another volunteer, came to the program with many years of nursing experience across clinical settings, including critical care, neurosciences, and outpatient women’s health.
My husband and I welcomed our baby girl on October 12—leaving just enough time for me to participate in the follow-up ultrasound experience on October 8. I am so thankful for the care and attention that the WHNP students showed me, and I can’t wait to see the kinds of nurse leaders they become!
Many people are called to nursing to care for young people. Some go on to become NICU nurses, others school nurses. Some become nurse scientists and tackle some of the most pressing issues facing youth today. There are countless nurses across the globe, and many here at Duke, focused on ensuring that children and adolescents have happy, healthy lives.
From Isolation to Support: How MASI Helps South African Adolescents Stay on HIV Treatment
Marta Mulawa, PhD, MHS, is a Duke scientist and assistant professor whose research centers on a practical question with life-long consequences: how to help adolescents living with HIV stay engaged in care and take treatment consistently. In South Africa—home to one of the world’s largest HIV epidemics—young people often navigate medication routines alongside stigma, disrupted support networks, and the everyday pressures of adolescence. But Mulawa also knows that youth across the globe often have one thing in common—whether it’s Chicago or Cape Town, they are never far from their mobile devices.
Those realities led Mulawa and her team to develop MASI, a comprehensive smartphone app designed to support young people living with HIV in South Africa with multiple features for day-to-day health management. MASI stands for Masakhane Siphucule Impilo Yethu, which is Xhosa for “Let’s empower each other and improve our health.”
A central design motivation was connection: the app helps adolescents link up with peers who may be facing similar challenges so they can better support one another. Mulawa’s prior work highlighted the power of peer influence in this population, and collaborators in South Africa emphasized that social isolation was a major and under-addressed barrier.
The project also built on existing digital health infrastructure. Mulawa worked with collaborators who had developed the HealthMpowerment (HMP) platform to support populations in the United States, creating an opportunity to adapt a proven approach to the needs emerging in South Africa. Because adolescents spend so much of their time on their phones, delivering support through a smartphone app aligned with how they already communicate and seek information.
What Adolescents Said They Needed—and How It Shaped the Design
In formative research, adolescents described a wide range of challenges that can derail consistent medication-taking—reinforcing the need for an app that supports multiple dimensions of adherence. One early, high-impact lesson involved information and messaging. Evidence in the HIV field shows that when someone takes treatment consistently and reaches an undetectable level of the virus in their body, they cannot transmit HIV to others—an empowering, destigmatizing message widely known as “Undetectable equals Untransmittable,” or U=U. Yet many adolescents in the study were not familiar with the concept or how it applied to their lives, meaning it was not serving as a motivator for adherence. As a result, sharing clear, empowering information about U=U became a key element of MASI, delivered directly through a medium adolescents engage with constantly and can revisit over time.
MASI is designed to complement clinical services, including through an “Ask the Expert” feature. Adolescents can post questions anonymously, which are then answered by a provider—one practical way nurses and other clinicians can support app use in routine care. Participants valued the ability to get answers to questions they might not have time to ask, or feel comfortable raising, in other settings.
Early Evidence: Feasibility, Acceptability, and Flexible Engagement
To test MASI, the team conducted a pilot randomized controlled trial with 50 youth living with HIV. The pilot demonstrated the app’s feasibility and acceptability, along with its potential to improve treatment adherence. Engagement varied across participants, but adolescents appreciated that MASI is comprehensive while still allowing users to pick and choose the content and features most relevant to their needs.
Supporting the Transition to Adult HIV Care
“Adolescents are in this unique development stage where they are beginning to more actively manage their own care and treatment,” Mulawa said. MASI offers features such as a “Health Tracker,” which allows users to scheduled tailored reminders and monitor how often they take treatment.
“We also have many activities and resources to support active self-management, which is critical as they transition into adult HIV care,” she added.
Impact and What Comes Next
Mulawa’s team has already seen preliminary, encouraging signals that MASI can improve treatment adherence. “The adolescents were very enthusiastic about moving forward to expand MASI to reach more youth and also to use it to address mental health challenges that they identified as a high-priority unmet need among adolescents with HIV in South Africa,” Mulawa noted.
By combining peer connection, trustworthy information, and low-barrier access to clinical expertise, MASI illustrates how digital tools can strengthen adolescent HIV care, and points toward scalable models that health systems can adapt to support young people over the long term. It’s nursing at its finest—combining clinical expertise and scientific knowledge to allow patients to not only survive, but thrive.
Empowering School Nurses to Meet the Youth Mental Health Crisis
Across the country, school nurses are becoming essential first responders in a growing public health emergency: the youth mental health crisis. With one in five students experiencing a major depressive episode each year, and nearly half receiving no treatment, the gap between student needs and available mental health services is widening. For her capstone project, Sahara Aguilar, DNP’25, RN, FNP-BC, investigated how school nurses (often the first adults to detect changes in students’ behavior, mood, or academic performance) occupy a uniquely influential position in addressing this issue; yet many feel underprepared, undertrained, and unsupported in navigating complex mental health concerns.
A New Model for Training: MHTIPS
Aguilar developed “The Mental Health Training Intervention for Health Providers in Schools” (MHTIPS), a training program that equips school nurses with practical tools for prevention, early identification, crisis response, and effective communication with students and families. Through a structured, multiweek training that blends self-paced modules with guided discussions and resource mapping activities, participants learn to recognize warning signs, deliver support, and navigate referral pathways with confidence.
Measurable Improvements in Knowledge, Confidence, and Preparedness
Results from the implementation are striking. Aguilar noted that nurses’ knowledge scores nearly doubled—from 43% pretraining to 84% immediately post training—and gains remained strong three months later. Confidence in discussing concerns, responding to crises, and referring students to services also rose significantly, with similar sustained improvement in preparedness across key skills such as recognizing distress, motivating students to seek help, and coordinating services. These outcomes reflected not only enhanced clinical competence but also the real-world impact, nurses reported; on average, they identified nearly a dozen mental health concerns in the months following the intervention, and 97% successfully connected students with needed resources.
A Promising Path Forward Despite Persistent Barriers
While participants in Aguilar’s program praised the relevance and quality of the training, systemic obstacles endure. “Insufficient staffing, restrictive policies, limited family engagement, and ongoing stigma continue to challenge school-based mental health efforts,” said Aguilar. Nurses who underwent the training called for more in-depth content, greater administrative support, and expanded resources to meet student needs effectively. Despite obstacles, the overall impact is unmistakable: MHTIPS not only strengthens the skills of individual practitioners but offers a scalable model for improving student mental health outcomes across diverse school settings.
Where Community Shapes Science
Across the School of Nursing, commitment to advancing health for all extends beyond individual patient care to a broader, holistic approach that recognizes the lifelong needs of diverse populations. Throughout work addressing the challenges of every stage of life, we embrace the vital role that collaboration with communities plays in fostering resilience, equity, and lasting well-being. By involving the communities we serve in every aspect of our work—from care delivery and education, to nursing science—we ensure that our impact is both far-reaching and deeply rooted, creating a foundation for health that spans generations.
Rosa Gonzalez-Guarda, PhD, MPH, RN, FAAN, knows firsthand the importance of community-engaged research. Dr. Gonzalez-Guarda has led a team of community members, researchers, PhD students, and nurse scientists in a years-long research program called SER Familia. SER Familia is a Duke University School of Nursing-led research program focused on improving the health and wellbeing of Latino immigrant families by addressing the combined effects of stress, social conditions, and health challenges.
Now in its second year, Dr. Gonzalez-Guarda reflects on the progress the program has made and looks forward to what comes next:
“In Year 2 of SER Familia, I found myself navigating a transitional phase—moving from protocol development to fully launching the study. This period was marked by initiating the project and actively refining processes to ensure fidelity, boost participant engagement, and keep us on track to meet our study aims. Our leadership structure has stayed strong, thanks to bi-weekly meetings with my fellow principal investigator (Dr. Richard C. Cervantes) and monthly check-ins with the entire investigative team.
"Throughout these meetings, my team and I have concentrated on building the infrastructure needed for high-quality delivery in community settings. We finalized the manual for community health workers (CHWs), prototyped a ‘return of results’ process that shares participant-specific profiles related to stress, resilience, and syndemic health, tested and refined our Research Electronic Data Capture (REDCap) platform for survey and process data collection, and completed procedures and instruments for fidelity monitoring and qualitative data collection. Altogether, these efforts have focused not only on launching recruitment, but also on standardizing and clarifying the intervention’s early touchpoints—especially Session 1, where CHWs use visual tools and interpretation guides to discuss baseline results with families.
"Preparing the workforce has been one of our biggest achievements. Starting October 23, 2024, our investigators and staff—led by Co-Investigator Irene Felsman, DNP, MPH, RN, C-GH and coordinators Ms. Garcia Ortiz and Zahira Decena—held weekly, two-hour sessions to train CHWs in research procedures, syndemic conditions targeted by the project, and best practices for implementing SER Familia. I also facilitated monthly meetings so I could stay closely connected to CHWs’ field experiences and surface implementation challenges they faced while working with Latino immigrant families. As CHWs began delivering the intervention, our meetings shifted from traditional training to structured supervision. During this time, nurses and other clinical team members—including public health practitioners and psychologists—provided consultative support for complex family needs that emerged, such as mental health symptoms.
Looking ahead to Year 3, my principal goals are all about scaling up while maintaining rigor: improving recruitment, enrollment, retention, and intervention delivery so we can get back on track with our original timeline (aiming for 80 dyads enrolled per quarter), supporting eight CHWs to recruit around 10 dyads each quarter with Duke staff pitching in as needed, advancing a protocol manuscript toward publication, and considering an administrative supplement to better capture implementation costs, challenges, and potential cost-effectiveness.”
Community-engaged research like SER Familia demonstrates the power of collaboration between academic institutions and the communities they serve. By centering the voices and experiences of Latino immigrant families, this work not only advances scientific understanding but also drives practical solutions that foster resilience and equity. As we move forward, continued partnership and investment in community-driven initiatives will be essential for creating lasting improvements in health and well-being.
The collective efforts underway at the School of Nursing—ranging from innovative data-driven initiatives like the NC SCDC to collaborative, community-engaged research exemplified by programs such as SER Familia—demonstrate the profound impact that our community, past and present, has on patients across the lifespan. By harnessing robust data systems, empowering community voices, and fostering meaningful collaborations, we move closer to nurse-led solutions that improve the lives of all people across the globe. At Duke we are weaving a tapestry of care that will touch generations with its impact.




